|
This is the second post in a series of blog posts introducing each member of the Summit Birth Utah team.
Through my first birth, I learned that patience and timing are everything and that cervical dilation is no indication of imminent birth. I was 7 cm dilated at 38 weeks, yet not in active labor. Not knowing what to do, I waited around to see if magically labor would start. When it didn’t, my husband and I were so anxious from waiting to see what would happen that we just went to the hospital. I was admitted, and interventions were thrown my way. My OB broke my water, then started me on pitocin, then I received an epidural. Fortunately, all went well and I delivered my healthy baby boy the next morning. The questions that keep swirling around my brain at those memories are: What if I had waited? What if I said no to the interventions? What if? Knowing that doesn’t help change the past, I’ve let those feelings simmer. Then my second birth happened later than I had hoped and expected. Being pregnant at 41 weeks is no walk in the park. I was anxious for my son to be born, since his brother made his debut 2 weeks early. Finally, we set an induction date when labor, once again, did not happen spontaneously. Again, my water was broken, pitocin was administered, and I received an epidural. This experience was different as the OB on call allowed me to pull my son out to my chest and I watched his gradual entrance into the world with the help of a mirror. It felt so empowering! But I knew there were choices I had left up to others to dictate how the labor went. That didn’t settle well with me either and again I had questions such as, “What if …?” I learned again that patience and timing are everything and I learned that there was much more to be understood about birth that I still didn’t grasp. The last thing I learned was that a medicated birth can also be a beautiful, wonderful, empowering experience. Then my third birth happened and I decided I wanted to try without the epidural and hoping upon hope I would spontaneously go into labor. Without a plan for how to handle the contractions, it was tougher than it needed to be. Labor stalled when we were admitted to the hospital and then I allowed my midwife to break my water. After that, things finally picked up. I tried hydrotherapy and then moved out of the tub as I went into transition. My husband and midwife did all they could for me as I reached completion. I don’t remember how long I pushed, but it wasn’t long before my beautiful daughter was placed in my arms. It was hard. I didn’t have the glorious, empowering feeling I had with my last birth. I was focusing everything on getting through the contractions, and without a guide, mind you. I learned that I should have prepared better and should have had a doula. Just a year after that birth, I found myself for the first time as a birth worker as I captured my nephew’s birth on camera. My sister, along with the staff, allowed me into the OR as she delivered her son via cesarean. With tears in my eyes, I photographed the emergence of my nephew from my sister’s belly. I couldn’t wait for the next birth. From there, I photographed many more births, each one filling my cup and my sense of awe for the wonder that birth is. I decided I lacked tools that would help me support women even more. I decided to make the jump and become a doula myself. I trained through CAPPA in 2020 with DoulaEd. I finally felt like I landed where I belonged. Empowering women through teaching them informed choices filled me with joy almost as much as motherhood fills me with joy. By the time I was pregnant with my fourth, I had a deeper grasp of childbirth, the stages of birth, comfort measures and the importance of knowing your choices and making informed decisions. I was so ready to take on this one (possibly final) challenge of birth and of making the choices that were best for me, my baby and my body. I took a childbirth education class from my doula. And yes, I hired a doula. Because of timing and circumstances, I chose to be induced. That wasn’t the first choice I had made. I was well-trained by that point, working with my health care providers as I navigated gestational diabetes, potential Intrauterine growth restriction, or IUGR, of my baby and choosing not to be induced sooner than was necessary. I already felt empowered before even stepping foot into the delivery room. With my induction, I was prepared to make even more choices, even though there were some restrictions. I felt my voice was heard and I labored how I wanted and then, when the time came, pushed how I wanted. I grasped the shoulders of my doula and husband, stood up on the bed and pushed and squatted my baby boy out into the world. It was incredible. I felt so strong and so capable.  That amazing birth experience gave me the strength I needed through my postpartum time. That first year was challenging, but because I knew I had already done incredibly hard things, I knew I could push through and endure these additional hard things. I’ll be forever grateful for my transformational birthing experiences. My hope is that every mom can have that same feeling from the births she has. My other hope is that every woman can feel the eternal pull of the divine role of motherhood. Motherhood is eternal and the joy we feel as mothers will continue beyond this life.  Before I became a mother to my four amazing children, I completed a bachelor’s degree in Communication from BYU-Idaho, served a full-time church service mission to Ecuador, and volunteered in Chile helping adults find employment. My husband and I met at BYU-Idaho and decided to become friends and lovers for life. We have been married for 15 years. I enjoy learning and reading, playing softball, and playing board games with friends and family.
0 Comments
This is the first post in a series of blog posts introducing each member of the Summit Birth Utah team. Hi, I'm Sara!
My StoryIt took me a while to figure out what I wanted to be when I grow up. I may even still be figuring it out. :) After high school graduation, I headed to college, thinking I would study English and get an editing minor, and would spend my career ridding the world of comma splices, bad grammar, and sentence fragments. After not too long, though, I decided I wanted to make a gentler, more inspiring impact on the world. I switched my major to Elementary Education and graduated with that degree. After teaching for a couple of years I realized something important about myself: I do not have the patience to manage the behavior of large groups of small children all day. At the end of my second year of teaching, I also gave birth to my twin daughters, which kept me busy for a while. :) Over the next few years, I did some private tutoring of elementary-age kids, but have not returned to classroom teaching. Around the time my son was born, I decided to go back to school again to get a master's degree in applied linguistics, emphasizing K-12 education for kids whose primary language is not English. I planned to go back to work as an elementary educator, but as an ESL specialist rather than a classroom teacher. That way, I reasoned, I could still inspire and teach kids, but wouldn't be responsible for a class full of kids. And I would be putting my love for language to good use! Then, my son was born, and everything changed. I fell hard for birth. I was smitten, twitter-pated. In love. My son's birth was the single most empowering and transformative event of my life. My twins' birth had been an emergency-laden medical event during which no one really recognized that I had a voice or preferences. It just happened to me. And, unfortunately, ended with an urgent c-section, which led to many other health complications for months and years afterwards. I prepared differently for my son's birth. I took a 10-week comprehensive childbirth class, and I knew my options. I chose a care provider who was supportive of them, and I had an unmedicated VBAC (vaginal birth after cesarean). I came away from that birth with a sense of wonder for my body and my strength. I wanted other women to experience birth this way. So I became a birth doula.
And then a postpartum doula, and then a childbirth educator. I used my applied linguistics MA to host a podcast and trainings for birth professionals about the power of our words. I planned for years on becoming a certified nurse midwife. But then, after five years of being a birth doula, I burned out from the on-call role of being available any time, day or night, for an unpredictable length of time. My mental health and family well-being called for a more predictable, daytime schedule. And I wasn't enjoying my nursing pre-requisite classes. I reeled for a while, wondering what I would do, when I had been so set on my dream of becoming a CNM. And then one day, I was driving my daughter to therapy, and she said, "You know, Mom, if you ever get tired of birth stuff, you would be a great therapist." That beautiful gift from my daughter started me on my current path. While I continue to teach childbirth classes and offer a postpartum support group, and I still manage this wonderful team of birth doulas, I am no longer practicing as a birth doula. I'm in school (again!) to become a mental health therapist, and I plan to specialize in perinatal mental health, serving clients struggling through infertility, miscarriage and loss, prenatal and postpartum mood disorders, and recovering from traumatic births. I love the twisty-turny path my story has taken, and it feels so good to be where I am now on this path. I am so grateful for all of the students and clients I have worked with over the years, and can't wait to see what comes next!  In traditional cultures around the world, strong traditions of postpartum food prevail: warm, easy-to-digest food is prepared for new parents as they recover from giving birth. In modern U.S. culture, we've unfortunately stepped away from the wisdom of many of these traditions. While some attention is given to prenatal nutrition, many new parents aren't given a word of counsel about how to feed and nourish themselves during the weeks following birth. (The textbook I consulted while writing this post had 12 pages of information about prenatal nutrition, and only 5 pages about nutrition and lactation, and didn't address general postpartum nutrition at all!) Giving birth is a whole-body process that affects every body system, including your digestive system! Being mindful about appropriate postpartum nutrition is crucial! Let's go over some essential nutrients to include in your diet during the weeks and months after giving birth. ProteinProtein plays an essential role in physical recovery postpartum. The main function of dietary protein is building and repairing tissue in your body. So if you had a perineal tear during your birth or you had a cesarean birth, it's especially important to have an adequate protein intake as you recover. Protein can also be lost from your body due to increased bleeding, inflammation, infection, and physical stress, so there's good reason to focus on prioritizing protein in your postpartum diet! As a general guideline (for all healthy adults, not specifically postpartum), protein should make up 10-35% of your daily caloric intake. If, for example, you eat 2,000 calories each day, 200-700 of those calories should come from protein. Another recommendation is that you eat 0.8 g of protein for every kg of your body weight. For instance, if you weigh 150 lbs, that is equivalent to 68 kg. 68 x 0.8 = 54.4, so you should aim to eat at least 54.4 g of protein every day. Protein also helps build up your immune system to keep you healthy while caring for your new baby! And protein plays essential roles in carrying nutrients throughout your body and balancing water and pH levels inside your body. So, what are some good sources of protein? Protein sources are categorized as complete or incomplete. Complete protein sources contain all nine amino acids that your body needs to carry out its functions. Complete protein foods include eggs, milk, cheese, meat, poultry, fish, and soy (which is the only plant-based complete protein source.) Incomplete provide some of the amino acids your body needs, but not all. Incomplete protein sources include grains, legumes (beans, lentils, and peas), nuts, and seeds. These protein sources need to be paired with a complementary protein source in order to meet all of your body's protein needs. For example, if you eat legumes and grains (think beans and rice) together, these two incomplete protein sources form a complete protein. Other protein combos that result in a complete protein include legumes and seeds (e.g. eating chickpeas and sunflower seeds in the same meal) and grains and dairy (e.g. whole-grain cereal and milk, or yogurt and granola). What's your favorite protein source? Do you prefer eggs, poultry, seafood, beans, or chickpeas? Are there other protein sources you love? Pick out a few favorites and keep them well-stocked! Vitamin CVitamin C is also an important nutrient that promotes healing and supports immunity. As you recover from giving birth and care for your baby, make sure to load up your diet with good sources of vitamin C! Some options include brussels sprouts, broccoli, bell peppers, kale, cantaloupe, mustard spinach, strawberries, oranges, and kiwi. ZincLike Vitamin C, zinc boosts your immune system and helps your body heal damaged tissue. As you recover from giving birth, be sure to include sources of zinc in your diet. Oysters are the best dietary source of zinc, so if you love seafood, enjoy some oysters! If oysters aren't your thing, all meats are high in zinc. For non-meat sources, nibble on some pepitas, almonds, or peanuts. Legumes like chickpeas and beans also provide zinc, and all of these foods are great sources of protein as well! Omega-3 Fatty AcidsPreliminary studies show that having sufficient amounts of omega-3 fatty acids (specifically DHA) is protective against postpartum depression. Omega-3s also increase mental focus and decrease inflammation. As a bonus, if you're lactating, high Omega-3 concentration in your milk will help your baby's brain and vision to develop! So, what are some good sources of omega 3 fatty acids? The most common source is fish (and fish oil supplements), including mackeral, salmon, herring, oysters, sardines, anchovies, and caviar. Not a fan of seafood? Flaxseed, chia seeds, and walnuts, are also good sources of omega-3s. You can also opt for omega-3 fortified eggs or dairy products or swallow a high-quality fish-oil supplement. IronIron stores can become depleted during pregnancy and birth, so the postpartum time is an important time to replenish your iron stores. It's estimated that 10-30% of postpartum women experience iron-deficiency anemia during the postpartum period. If you have symptoms of iron deficiency, such as fatigue, depression, and altered cognition (memory loss, trouble concentrating or understanding), be sure to see your medical care provider to monitor your iron levels. As a guideline, though, everyone should prioritize iron during the first months postpartum. Iron-rich foods can be found in most food groups: most meats are good sources of heme iron (beef, ham, turkey, chicken, pork, etc.), as are eggs. Many seafoods provide iron, including shrimp, tuna, oysters, clams, and mackerel. Vegetables and fruits can provide non-heme iron, too! Non-heme iron isn't absorbed by your body as easily, so you need to eat more of these plant-based iron sources. Load up on spinach, sweet potatoes, peas, broccoli, strawberries, watermelon, prunes, dried apricots, and more! Whole-wheat and enriched grains also provide iron, and tofu, beans, lentils, and blackstrap molasses are other sources. And cooking in a cast-iron skillet boosts your iron intake as well! Wrapping it UpAfter you give birth, there are so many demands that pull on your time and energy, primarily your sweet new baby! But remember, that you, too, are being reborn. Take time to care for yourself and your physical body as you recover and adjust during the postpartum period. Fuel up on foods that will replenish your body--it's one way to tell yourself that you matter, too! ReferencesCpt, M. G. M. R. (2022, June 24). Postpartum nutrition: A guide to healthy eating after giving birth. Nutrisense Journal. https://www.nutrisense.io/blog/postpartum-nutrition-eat-healthy-after-giving-birth
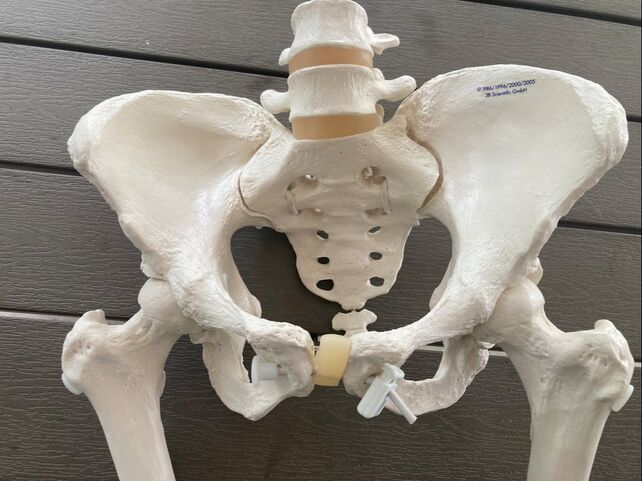
Leung, B., & Kaplan, B. (2009). Perinatal Depression: Prevalence, Risks, and the Nutrition Link—A Review of the literature. Journal of the American Dietetic Association, 109(9), 1566–1575. https://doi.org/10.1016/j.jada.2009.06.368 Lindberg, S. (2020, July 31). Postpartum diet plan: Tips for healthy eating after giving birth. Healthline. https://www.healthline.com/health/postpartum-diet#guidelines Reinagel, N. D. M. (2024, February 20). Top 5 nutrients for Postpartum recovery. Scientific American. https://www.scientificamerican.com/article/top-5-nutrients-for-postpartum-recovery/ World Health Organization (2016). Iron Supplementation in postpartum women. [PDF]. In WHO Library Cataloguing-in-Publication Data. https://iris.who.int/bitstream/handle/10665/249242/9789241549585-eng.pdf?sequence=1 Yahya, N., Teng, N. I. M. F., Das, S., & Juliana, N. (2021). Nutrition and physical activity interventions to ameliorate postpartum depression: A scoping review. PubMed, 30(4), 662–674. https://doi.org/10.6133/apjcn.202112_30(4).0013 The first time I ever visited a chiropractor, I was 36 weeks pregnant. I'd been waking up for my middle-of-the-night bathroom breaks with SO much pubic bone pain that I had to wake my husband to help me walk the five feet to the bathroom. I waddled into her office in Cambridge, Massachusetts, feeling very pregnant, very uncomfortable, and very desperate. At the end of my appointment, I stood up and walked to the door. I realized that, for the first time in weeks, I wasn't doing my pregnant waddle! I was SO much more comfortable. My pubic bone discomfort (symphysis pubis dysfunction, also called SPD or pelvic girdle pain) was minimal. I visited her for the last few weeks of my pregnancy and was extremely grateful for her specialized care. And I'm certainly not the only prenatal chiropractic success story! A doula friend of mine had a client who had been in early labor for three and a half days. She was having contractions, but they just weren't forming a pattern to lead to active labor, opening of her cervix, and birth of her baby. On day four of early labor, she went to a chiropractor (the fabulous Dr. Nick Shelton at Shelton Chiropractic in Salem, UT), and within five minutes of her appointment, her contractions were strong and regular. Her baby was born 6 hours later! When I asked for prenatal chiropractor success stories in a birth group on Facebook, my post was flooded with comments. One mom said, "My chiropractor knew I was working hard for a VBAC so he was a key part in that for me. I saw him weekly my entire pregnant and it always gave me some relief from the pregnancy related aches. Then in my last 8 weeks, he saw me twice a week and would focus more on adjusting my hips so we could get the baby in a good position. The consistency of my visits not only helped me stay active my entire pregnancy but I also had a very smooth delivery and a successful VBAC! I completely credit a part of it to my chiropractor." Another mom shared her story of how she'd barely been able to walk due to SI pain (pain at the sacroiliac joint, where the spine joins the hips). She visited Timpview Chiropractic in Orem, UT. After chiropractic care, she was able to walk and stay active during the rest of her pregnancy and birthed a 9 lb baby! Still another mom shared how uncomfortable she'd been during her pregnancy, suffering from general pain and sciatic pain. Her chiropractor was able to reduce her general pain and eliminate her sciatic pain. Now pregnant again, she's made regular chiropractic care at Renegade Chiropractic part of her self-care, and she's able to stay active as a student, at work, and as a mom. There were too many stories shared for me to recap all of them here, but I'll share one last story about how a chiropractor was able to help a client have a successful VBAC: "My chiropractor is the reason I was able to have a VBAC. My baby in a sunny side up orientation was no match for stalled dilation; but once my chiropractor adjusted my back, and aligned my hips, my baby was able to drop and rotate into a more optimal position. I labored for 26 hours, got adjusted, and had our baby 90 minutes later at the birth center." Why is prenatal chiropractic care so effective?At this point, you're probably thinking, "are they magic? How are chiropractors so effective at minimizing pain and speeding up labor?" During pregnancy, labor and birth, your baby descends into your pelvis. The pelvis is, in my opinion, the coolest-shaped bone in the body. Check it out: Technically, it's two bones: the ossa coxae (singular: os coxae), that meet the sacrum (the large bone at the base of your spine) in the back, your left and right femurs (thigh bones) on each side, and come together at the pubic symphysis in the front. Along with the muscles of your pelvic floor, your pelvic bones are responsible for holding much of the weight of your growing baby and body throughout pregnancy. As your baby grows and your body accommodates baby and grows as well, sometimes the pelvis can get a little out of whack, or misaligned, as chiropractors would say. Your spine can also get misaligned during all of this growing and stretching. One way chiropractors work their magic is by re-aligning any misalignments in your spine and pelvis, which in turn helps your whole body work together more effectively. This also creates optimal space for baby to rotate and descend during labor and birth. This is not my field of expertise, so from here, I would invite you to reach out to some of my favorite chiropractors serving Utah County who specialize in care during pregnancy. They are also great resources for pediatric chiropractic care and see kids as young as newborns! Recommended Prenatal Chiropractors
Other ResourcesIf you're looking for a prenatal chiropractor in your area or more information about chiropractic care during pregnancy or for infants and kids, check out ICPA or Utah Pediatric Chiropractors. For more amazing resources about physiological birth and how your positioning, alignment, and body balance impact your comfort during pregnancy and your baby's descent during labor, check out Spinning Babies.
Wishing you a well-aligned pregnancy and birth! By Eliza Payne Imagine this: You are a few days past 40 weeks of pregnancy, excited to meet your sweet baby. Just as you are getting ready for bed and notice some cramp like sensations, more intense than the Braxton Hicks contractions you often experience. You are filled with excitement thinking, “Could this be the start of labor?” As you continue getting ready for bed you notice the sensations last about thirty seconds and come every 15 or 20 minutes. Is this early labor? What do you do now? Sometimes it’s hard to tell at first if what you are experiencing is really labor - and that’s okay. Early labor offers an invitation to embrace the mystery and unknown of how and when your baby will make its way earthside. There is usually a slow, gradual process of contractions becoming longer, stronger, and closer together. Every labor has its own unique unfolding, but often early labor is the longest phase of labor. So what are some of the most helpful things to do during this time? Here are a few suggestions for early labor: 1. Practice patience. As you feel those first contractions, you never know exactly how much longer it will be until you hold your baby in your arms. You could be in labor for a few hours or a few days. One of the most helpful things to remember is, labor takes as long as it takes. I know it’s hard when you are excited to meet your baby, but early labor often requires a lot of waiting and patience as you let things unfold in their own timing. Try not to rush or force things to happen and practice patience instead. 2. Ignore labor until you can’t anymore. Similar to practicing patience, ignoring labor early on can help your mindset immensely. If you focus a lot on contractions too soon it can be emotionally and mentally exhausting. Try to go about your activities like normal, without thinking too much about being in labor or how long it has been. Distraction can be really beneficial at this point. 3. Rest, rest, rest!!! Especially if early labor starts in the middle of the night, try to sleep as long as you can! If you are about to go to bed and contractions are mild, try to sleep! If it is the middle of the day, try to take a nap! Do you get my point yet? Always try to rest, even if you don’t actually sleep. Restful activities will help conserve your energy so you have more of it when you need it most towards the end of labor. Some people enjoy working on a relaxing labor project alone or with their partner, like baking a special treat or working on a puzzle that you saved just for labor. A few more restful ideas: take a bath, get a massage, watch a show, read alone or with your kids, recline with your eyes closed, or listen to a meditation, calming music, an audio book or podcast. 4. Stay hydrated and eat something. Labor is an extremely physical event and your body needs plenty of fuel. Focus on staying hydrated and eating in early labor because it might be the last time you get a good meal for a while. Electrolyte beverages are especially helpful, such as coconut water, Gatorade, or homemade labor-aid (you can look up recipes online, but recipes usually include coconut water, fresh lemon juice, sea salt, and honey). Bone broth is another nourishing option. As for food, focus on high protein, healthy fats, and complex carbs to keep you full and energized. Listen to your body and eat what sounds good. 5. Create an oxytocin-rich environment. Oxytocin, the love hormone, plays a key role in labor. It can help with labor progression and also acts as a natural pain reliever, so it is essential to keep the oxytocin flowing in early labor. Try to decrease stress as much as possible and increase oxytocin by creating more love in your environment. Think cuddling, sex, massage, slow dancing with your partner, listening to music you love, watching a funny show, eating foods that bring you comfort, or anything that makes you happy and feel loved. 6. Try not to engage your thinking brain. As you go through labor, brain waves change and become increasingly slower and drop into a more primal, feeling state. To help your mind relax, try to avoid new environments that require a lot of thinking, talking, or social interactions. If the weather permits, you might enjoy being outside and connecting with nature. Try going inward and tune into your body. Don’t focus on the clock or timing contractions. Ask your partner to take care of any logistics, like last minute packing or securing childcare, so you can go deeper into a relaxed, meditative state. 7. Move intentionally. If you have rested all you can, have the energy, and are practicing patience and not trying to rush labor, there can be some really helpful movements and positions for early labor. Doing the Miles Circuit or Spinning Babies Three Balances can be very helpful to get your baby in an optimal position for labor. Any kind of gentle movement, like figure eights on a birth ball, pelvic rocks, or walking can be beneficial. Just remember not to over-do it and wear yourself out. Your energy is precious and you will likely need a lot of it later on. 8. Stay at home as long as possible. Especially if your goal is an unmedicated birth, it is a good idea to stay at home as long as possible. In early labor your baby does not need to be monitored and it is better for you to be in the comfort of your home where you can get in a good rhythm without the constant interruptions from the medical staff. Often things can progress faster at home because you can more easily incorporate all of the suggestions above. After all, when you are at home it is easier to stay patient, ignore labor, rest and relax, eat and drink, create more oxytocin, not be in your thinking brain, and move intentionally.
Early labor can be a time between worlds and you may experience a range of feelings, from excitement and nervousness. All the months of waiting and preparing for your birth have led to this moment. In the coming hours or days, you will soon be meeting your baby! Hopefully some of these tips can make your labor more of a positive, empowering experience where you discover your strength. Preparing for a new baby can be expensive, and the list of things you could spend money on during your pregnancy can seem endless! Childbirth education can be a bit of a financial investment, but taking a high-quality childbirth class is worth every penny! Here's why: 1. You'll feel so much more prepared and confident going into your birth.Knowledge is power! Especially if this is your first time giving birth, there's probably a lot you don't know yet about the physical, physiological, and emotional process of giving birth. Many first-time parents who don't take a class feel overwhelmed by all of the unknowns during the birth process and end up second-guessing their decisions and having a less-than-ideal experience. (I speak from my own experience and from the experiences of many clients who came to me wanting a better experience for their second birth.) 2. You'll connect with other parents-to-be.Taking a group birth class is a great way to connect with others in your same life stage! The people you meet in your birth classes could become some of your close friends, and will be great options for play dates as your kids grow! This goes for both moms and dads. Our childbirth classes are designed for both parents to attend, so you'll have a chance to meet other dads and moms who "get it." Making the transition to parenthood can feel lonely if your friends are in different life stages, so birth classes are a great chance to make new friends who are celebrating the same milestones and facing similar challenges as you! 3. Trained childbirth educators will share the info that really matters in a way that you'll remember it.We get it. There's SO much info on the internet and social media apps these days. It's tempting to think that you can get all the information you need to prepare for childbirth on your phone or computer. There's a huge benefit, though, to having an expert childbirth educator facilitate your learning. After spending some time following Instagram accounts and searching Google, you'll quickly discover that there's WAY more info on the internet about birth than you could ever hope to learn during your pregnancy. And some of it seems contradictory! Taking a childbirth class means you have an experienced, knowledgeable teacher who has mined through all of the childbirth information and found the most important content to share with you. And if you take a birth class through Summit Birth Utah, we can guarantee that our classes will be memorable and engaging... way more fun that scrolling on your phone!
WelcomeWelcome to the journey. Whether this is your first baby or your fifth, your pregnancy marks the start of a new path on your journey of motherhood. As birth professionals, we've walked this path before. We have the knowledge, skills, and experience to help you prepare for and enjoy a positive and empowering birth. We love birth. Like hiking to a mountain's summit, giving birth pushes us past our perceived limits. It urges us to call on our inner strength and climb to new heights. And the journey's pinnacle, as we snuggle our new little babes to our skin, rushed with hormones that fill us with indescribable love, is truly life-changing. It's empowering to look back over the ascent and its challenges and say, "we did it!" Discover Your StrengthThe Summit Birth Utah tagline is "discover your strength." Childbirth is unlike any other human experience. When else do we go to the edge of what we thought we were capable of, persist through and past it, and bring forth new life? Sometimes, the magic and wonder of birth are lost to beeping machines and hospital gowns. But no matter how or where you give birth, the act of bringing new life into the world is incredible. You are incredible. And we hope that, through this experience, you are able to discover new strength within yourself. We hope that, through birthing your child, you also rebirth yourself. You are so much stronger than you know. And birth can help you discover your strength. Thoughts from the Summit Birth Utah Team"We can go our entire life feeling like we know who we are, and what we are made of, but it’s not until you experience the incredible opportunity of creating a unique individual inside of you, and bring that child into the world that you truly discover the depths of your own strength. During those incredible moments, you experience innate inner strength on a level that could not be adequately described to you, but must be experienced to comprehend. The cries of a woman delivering a child are some of the most beautiful sounds in the world. I am woman, hear me roar!" -Esther Whitney "I discovered my strength when I was giving birth to my fourth child. I was at the point of pushing and I felt like I just couldn't do it. I didn't WANT to do it; it was too hard! But thanks to my midwife and my doula, they reminded me that I have the strength to do it, to push my baby out. Only I could do it. And guess what? I did! I remember distinctly summoning the courage, taking a breath and pushing my little boy out and into this world. It was the most amazing thing." -Sarah Roberts "Birth is a brave journey into the unknown that requires mental, physical, and emotional strength. I have witnessed this strength in every woman who has risen to the challenge of giving birth. Sometimes this means facing fears, advocating for needs, processing difficult emotions, coping through intense contractions, or simply being present with what is. Even -maybe especially - when things don’t go as expected, strength is found as you carry on and face the unknowns of birth." -Eliza Payne "In pregnancy and birth we are at our most vulnerable and, in that, our most powerful. There is a particular and deep strength inside us that can only be accessed in doing the intense, instinctual, and incredible work of bringing a soul to life. That strength is there in every birth, but sometimes can be masked by many different dynamics that can accompany birth. When we are educated and supported, we can truly discover (and use, and celebrate!) our powerful strength."
-Charity Eyre Wright Are you thinking of hiring a doula? Or just curious about what exactly a doula is? Maybe you want to take a childbirth class, but you’re overwhelmed by all of the options and not sure which one is the best fit for you.
To help you find answers to these questions, Summit Birth Utah is hosting a FREE Virtual Meet & Greet! Join us on Zoom on Tuesday, Aug. 1 from 8:00-8:30 PM MDT. Register here to get the link! If you're not sure you can make it, you can register anyway, and we'll send you a recording of the Meet & Greet afterward! Here's what to expect at this FREE event: For the first ten minutes, each member of the Summit Birth Utah team will introduce herself. We have three incredible birth doulas: Eliza, Esther, and Sarah, and two fabulous childbirth educators: Charity and Sara. Each team member will introduce herself, sharing her background, why she loves birth work, and some logistics about the area she serves/the class she teaches. Then, we'll answer questions that were sent in from registration forms and social media polls before the event. You'll hear answers to questions about the services we offer, our grant program for families with financial constraints, and your questions about pregnancy, birth, and the postpartum time period. For the last several minutes, we'll open it up for questions from live participants. This is a big perk of attending live! Based on what you've heard from the first two-thirds of the Meet & Greet, you can ask follow-up questions or anything that has popped into your head. Take advantage of having five experienced birth professionals at your fingertips, and pick our brains! After the official end of the 30-minute event, we'll turn off the recording and stay on the call for a while longer if you have questions you'd rather ask off-record or more privately. (We'll even send you to a private virtual breakout room with a member of the team if that's most comfortable for you.) We know that pregnancy and birth can be intimate, vulnerable topics, so we'll provide a respectful space for you to ask your more private questions. After 15-20 minutes for non-recorded questions, we'll call it a wrap! We hope you'll join us for our FREE Virtual Meet & Greet! And please share this post with the other expectant parents in your life! If you're a parent-to-be researching adding a doula to your birth team, you may have asked this question. Depending on your area and the experience level of your doula, a complete doula services package is typically $1,000-$3,000. That can feel like a big investment! But I guarantee, an excellent doula is worth that much (and more)! In order to understand a doula's value, it's important to first know what a doula is. If you're not quite sure, read this post for a detailed explanation, and then head back here to keep reading! In addition to the physical, emotional, informational, and relational support outlined in the "What is a Doula?" post, doulas do so much behind-the-scenes work that adds value to what they offer as a member of your birth team.
In addition to all of this value that doulas offer to their clients, consider how doula support can be an investment that ends up saving you money in the long run!
Ideas: How to Afford a DoulaI'm hoping, by now, that I've convinced you that doulas are well worth the doula package price of $1,000-$3,000. Even so, it may still feel out of reach for you to hire a doula. What can you do?
You may need to think outside the box a little, but there are definitely ways to make having a doula a possibility for you! Here are some ideas:
Sometimes, even with all of these ideas, hiring a doula may still feel unreachable for you. If finances are tight and the above ideas aren't working for you, or aren't reaching far enough, please fill out an application for a grant for birth services. We offer grants of various sizes based on client need and current grant fund balance. We're typically able to offer at least a small grant (and sometimes a very substantial grant) to everyone with true need who applies! At Summit Birth Utah, we truly believe that everyone deserves a supported birth, and we will do everything we can to make doula support a possibility for you.  Have you ever wondered what exactly a birth doula is and why people choose to have them as part of their birth team? A birth doula serves as a trusted companion, offering physical, emotional, informational, and relational support throughout your pregnancy, labor, and postpartum period. Physical Support During labor, birth doulas offers techniques and guidance to help manage discomfort and promote optimal positioning. They may suggest comfort measures, provide massage, and use relaxation techniques to alleviate tension. Emotional Support Pregnancy and childbirth can bring up a range of emotions, and birth doulas understand this. They offer a nurturing presence, a listening ear, and words of encouragement to uplift and empower you. Informational Support Equipped with evidence-based knowledge, birth doulas share the information necessary to make informed decisions regarding your birth preferences. They provide resources, answer your questions, and help you understand the various options available, empowering you to actively participate in your birthing journey. Relational Support As a valuable member of your birth team, birth doulas work collaboratively with your healthcare providers, partner, and support network. They facilitate open communication, ensuring that your needs and preferences are respected and understood. Would you like to hire a birth doula to experience all of these benefits? We have a team of three fabulous birth doulas serving Utah County and Salt Lake County. All of our doulas offer free consultations, so you can find the right fit for your unique personality, needs, and values. We believe that everyone deserves a supported birth, so we also offer grants for families with financial constraints. If you would benefit from this, visit www.summitbirthutah.com/grants to fill out an application! Share this post with others who may benefit from understanding the invaluable role of birth doulas. Together, let's spread awareness and support for positive and empowering birthing experiences! |
AuthorHi, I'm Sara. I'm the founder of Summit Birth Utah! I'm a twin mom (plus one!), natural VBACer, and birth lover! Archives
May 2024
Categories
All
|





























 RSS Feed
RSS Feed